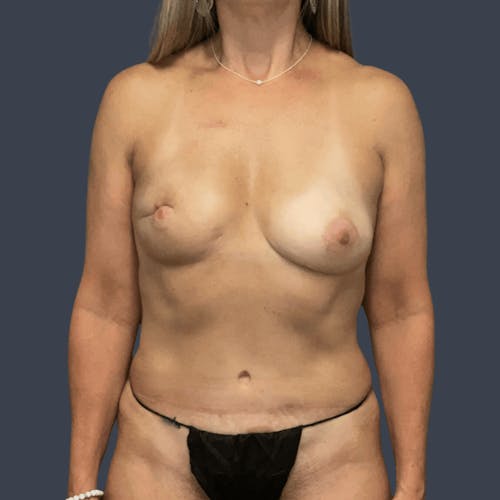
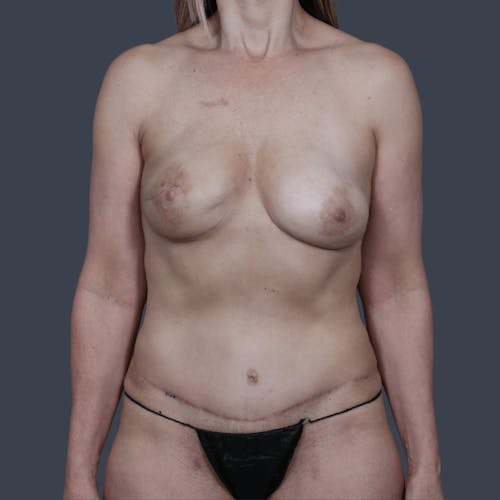
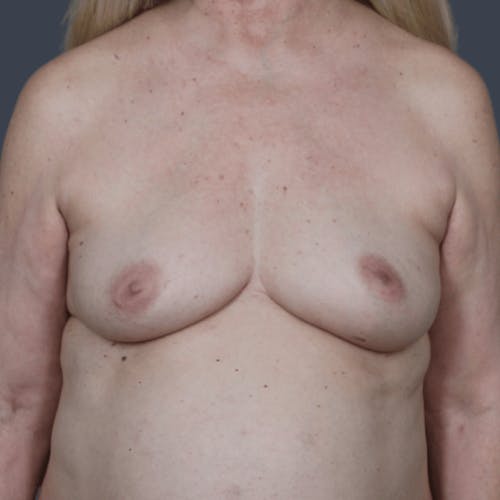
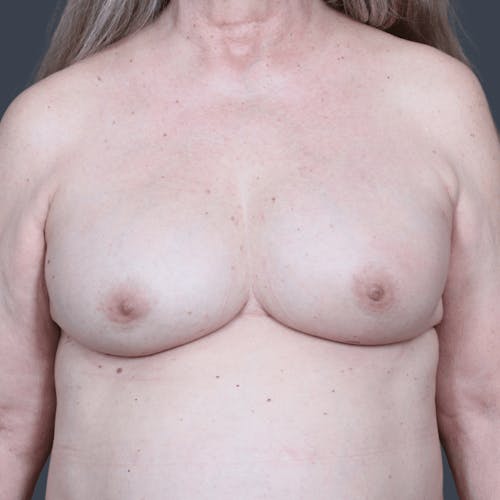
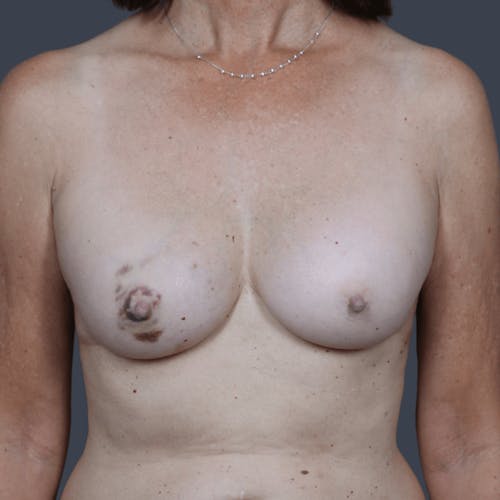
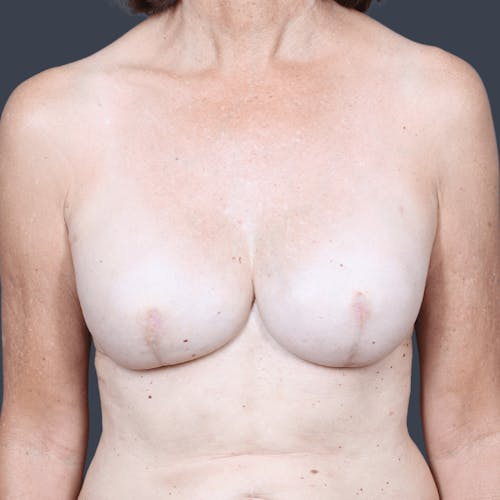
The decision to reconstruct a breast after cancer is a highly personal one. Women who choose to take this step are on a journey to recovery, and reconstruction is often a step that brings psychological healing and restoration of a woman's self-confidence. The importance of this process should not be underestimated. Choosing a reconstructive plastic surgeon with a special focus on the full range of breast reconstruction options is imperative to ensuring a positive experience and a superior outcome.
Our reconstructive plastic surgeons are an all-female team who have extensive experience working with breast cancer survivors to provide aesthetically beautiful reconstructive outcomes. To help our patients feel whole once more, our surgeons work closely with each patient—as well as the patient's surgical oncologist and medical team—to create a surgical plan that will meet the patient's needs and expectations best, as well as safely address the cancer. There is no one-size-fits-all approach when it comes to breast reconstruction.
Experienced in a broad range of techniques, our reconstructive surgeons are uniquely qualified to help women achieve beautifully natural results through reconstructive surgery. Whether you choose a flap technique that uses tissue from your own body or opt for an implant-based breast reconstruction, our surgeons will work to ensure your outcome meets your expectations and your desired results. For some patients, a combination of the two techniques may be used to produce the best possible results.